
Medically Reviewed by Stuart Wasser, MD and Samantha Callister, LCSW
Last reviewed:
Dual Diagnosis Treatment Long Island
01 · The Basics
What Is Dual Diagnosis Treatment?
Co-occurring substance use and mental health conditions, treated as one.
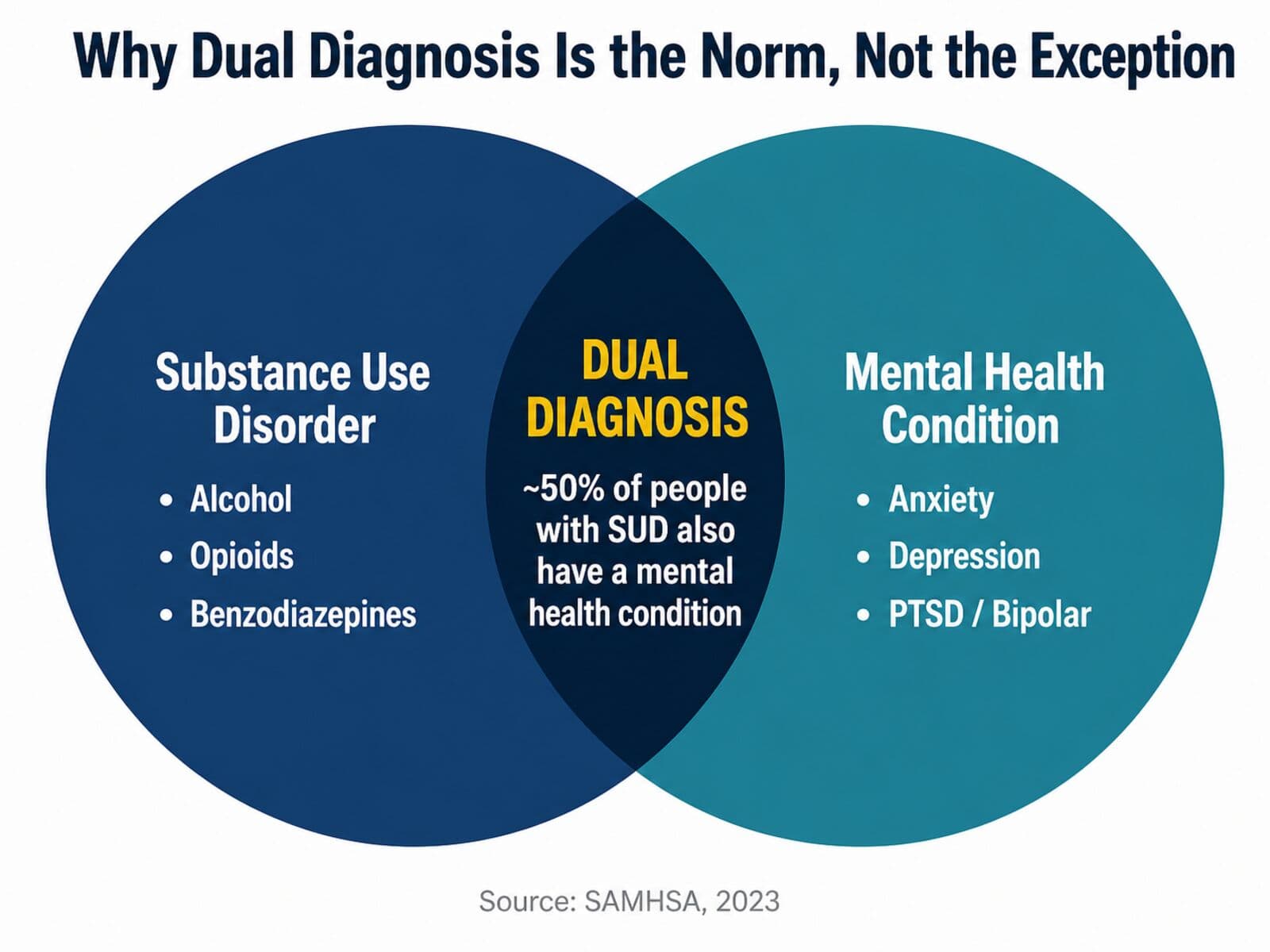
Dual diagnosis (clinicians usually call it co-occurring disorders) is when someone is dealing with a substance use disorder and a mental health condition at the same time. Anxiety. Depression. PTSD. Bipolar. About half the people with a substance use disorder are also living with one of these, and the two feed each other.
Dual diagnosis treatment handles both at once, in one plan, with one team. That sounds obvious, but most programs still don’t do it — they treat the addiction first and refer the mental health side out, which is why so many people relapse. At Integrity, dual diagnosis is the default, not an upgrade.
Most clients get this care through our Long Island IOP for dual diagnosis: 9 to 15 hours a week, with psychiatry and substance use therapy on the same schedule.
02 · Conditions
Conditions We Treat Together
Six co-occurring conditions, one integrated team.
Anxiety & Panic Disorders
Anxiety & Panic Disorders
Anxiety treatment for Long Island clients combines CBT, exposure work, and non-addictive medication options when appropriate. We see GAD, panic disorder, and social anxiety regularly — often as the underlying driver of alcohol or benzodiazepine use.
See benzodiazepine addiction treatmentDepression Treatment
Depression Treatment
Depression treatment in Nassau County uses behavioral activation, CBT, and psychiatric medication management. Our psychiatrists screen for and address bipolar depression specifically — misdiagnosed bipolar is a common reason “depression treatment” doesn't work.
Schedule a depression-and-addiction intakePTSD & Trauma-Informed Care
PTSD & Trauma-Informed Care
Trauma is one of the strongest drivers of addictive behavior. Our trauma-informed clinicians use EMDR, CBT for trauma, and somatic approaches alongside addiction work — never on top of it. We don't ask you to choose which problem to solve first because they're the same problem.
More on trauma-informed care belowBipolar Disorder & Substance Use
Bipolar Disorder & Substance Use
Bipolar I, bipolar II, and cyclothymia each need different medication strategies. We coordinate psychiatry and substance use treatment so mood stabilization and recovery happen together, not in series.
MAT options that coordinate with mood stabilizersSchizoaffective Disorder & Substance Use
Schizoaffective Disorder & Substance Use
Schizoaffective disorder pairs mood symptoms with psychotic features. Our outpatient program coordinates antipsychotic and mood stabilizer management with addiction therapy in our IOP. Best for clients who are medication-stable and working with an established psychiatric provider — we coordinate care, we don't replace primary psychiatric oversight.
Talk to our intake team about coordinated careSchizophrenia & Substance Use
Schizophrenia & Substance Use
Schizophrenia and substance use co-occur in roughly half of cases. Our outpatient program serves clients who are medication-stable and have a primary psychiatric provider. We provide integrated addiction therapy that coordinates with — never replaces — psychiatric care. Active psychotic episodes need a higher level of care first.
Verify fit with our intake team
“Half the people I see for addiction also have a co-occurring mental health condition driving it. If you treat one without the other, you’re treating neither.”
03 · Your Team
Meet Your Providers
Board-certified addiction medicine. On-staff psychiatry. Real names.
04 · Levels of Care
You Don’t Need to Be Admitted
Most Long Island dual-diagnosis programs are inpatient-only. Most people don't need it.
Inpatient / Residential
- Leave home for 30 to 90 days.
- Quit your job or take leave.
- Step away from your kids and partner.
- Re-entry shock when you discharge.
Outpatient + IOP
- Sleep in your own apartment.
- Keep working — day and evening tracks.
- See your kids, partner, dog every night.
- Same medical team, same evidence base, no re-entry cliff.
Insurance
Covered by Major Insurance
We verify your benefits before your first visit. Coverage and out-of-pocket cost depend on your specific plan.
- ♥ healthfirst
- New York Medicaid
- ≡ MEDICARE
- Fidelis Care
- MagnaCare
- + most commercial plans
05 · Approach
Trauma-Informed Care
EMDR, CBT for trauma, and somatic work — alongside addiction, never on top of it.
A lot of addiction is unhealed trauma. You don’t have to pick which problem to solve first — they’re the same problem. It also shapes the day-to-day: predictable session structure, consent at every step, and clinicians who can tell when a memory is being processed versus avoided.
EMDR Therapy
Eye movement desensitization for trauma processing.
CBT for Trauma
Cognitive restructuring around traumatic memory.
Somatic Approaches
Body-based work for stored trauma response.
06 · How to Choose
What to Look For in a Program
Six criteria that separate a best-in-class Long Island program from a brochure.
| What to Look For | Typical Program | Integrity Treatment Partners |
|---|---|---|
| Integrated medical + therapy team, same week | Separate referrals, no shared notes | One team, same week, one care plan |
| Board-certified addiction medicine physician on staff | Rare — usually a consulting referral | Yes — Dr. Stuart Wasser, MD |
| Joint Commission Accredited | Roughly a third of LI providers | Yes |
| Outpatient option (stay home, keep working) | Often inpatient-only or partial-day | Yes — IOP and standard outpatient |
| In-network with Medicaid + Healthfirst | Limited — many private programs decline | Yes — plus Medicare, Fidelis, MagnaCare, most commercial |
| Verifiable, published client reviews | Hidden or scrubbed | 4.9★ on Google · 146+ reviews |
Comparison reflects publicly available program information for Long Island dual-diagnosis providers as of 2026. Verify current insurance status, accreditation, and physician staffing directly with each program.
07 · The Models
Integrated vs Sequential Treatment
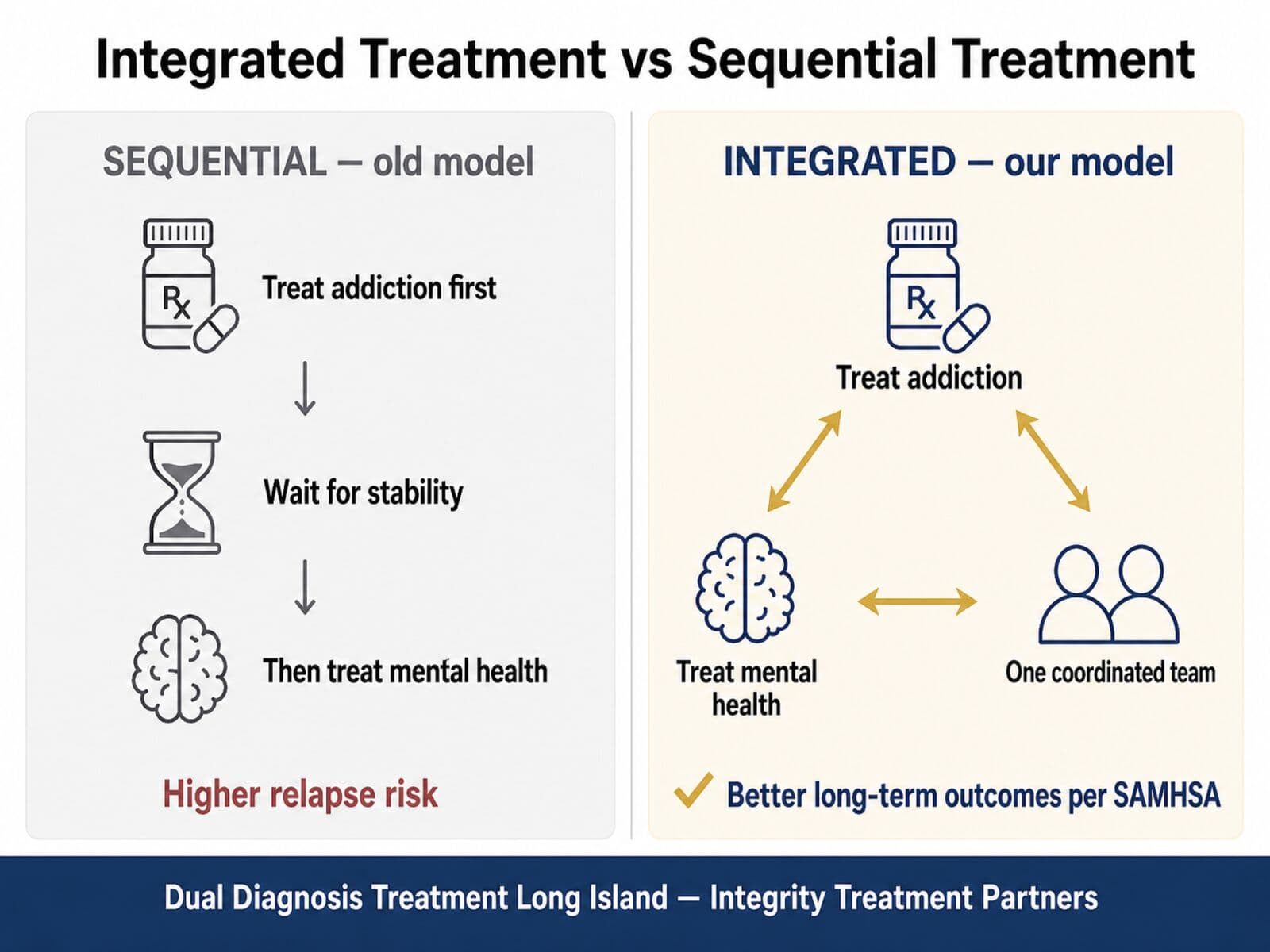
Why one model causes relapse and the other prevents it (per SAMHSA).
Sequential Treatment (old model)
- • Treat addiction first, mental health later.
- • Two providers, two plans, no shared notes.
- • Mental-health symptoms drive relapse before stabilization.
- • Higher relapse rates.
Integrated Treatment (our model)
- Both treated the same week, by the same team.
- One coordinated care plan across psychiatry and addiction medicine.
- Mental-health stabilization protects sobriety.
- Better long-term outcomes per SAMHSA guidance.
Source: SAMHSA — Co-Occurring Disorders and Other Health Conditions.
08 · Programs
Dual Diagnosis IOP on Long Island
9 to 15+ hours a week. Day or evening. Sleep at home.
Most of our Long Island dual diagnosis clients do their treatment through our Intensive Outpatient Program. The psychiatrist and the addiction therapist are on the same weekly schedule, in the same building. Enough hours to actually treat the mental health side. Not so many that you have to put your life on pause.
Day track or evening track. You can hold a job, pick up the kids after school, sleep in your own bed. Most people step down to standard outpatient at 8 to 12 weeks — once the meds are dialed in and the weekly schedule feels routine.
Long Island IOP for Dual Diagnosis
09 · The Process
How It Works
From assessment to medication to weekly therapy — one team, one schedule.
Full Assessment
Psychiatry + addiction medicine in the same intake. One unified plan.
Medication Management
Psychiatric meds coordinated with MAT. No conflicting prescribers.
Integrated Therapy
Individual + group sessions that work both conditions together.
10 · Coverage
Towns We Serve
Anxiety, depression, PTSD, and bipolar dual diagnosis treatment for Nassau and western Suffolk. Virtual care statewide.
See all Long Island locations we serve for outpatient and dual diagnosis treatment.
Same-Day Intake & Admission
Available Monday through Saturday. Insurance verified before your first visit — Healthfirst, Medicaid, Medicare, Fidelis, MagnaCare, most commercial plans.
Understanding Dual Diagnosis Treatment
Watch this video to learn how integrated dual diagnosis treatment addresses both addiction and mental health conditions together.

Ready to Start Your Recovery?
Call us today to schedule your intake. Our compassionate team is here to help you take the first step toward recovery.
Serving Nassau, Queens, Suffolk, and Westchester Counties
Integrity Treatment Partners provides outpatient addiction treatment and mental health services to residents across Nassau County, Queens County, Suffolk County, and Westchester County. The town pages below focus on the nearby Nassau County communities closest to our Baldwin location:
For county-level coverage and current virtual-service availability, view Integrity Locations.



